Sven Putnis offers expert realignment osteotomy surgery in Bristol. Discover advanced joint-preserving treatment for osteoarthritis driven by leg bowing.
Realignment osteotomy is a highly specialised, joint-preserving surgical procedure designed for patients with moderate to severe knee osteoarthritis that is driven by an abnormal bend or “bow” in the leg. When a leg is bow-legged (varus) or knock-kneed (valgus), it places excessive, uneven pressure on one side of the knee joint, accelerating cartilage wear. Instead of replacing the joint, an osteotomy involves making a precise surgical cut in the bone to correct this alignment.
By shifting the body’s weight away from the damaged, arthritic area and onto the healthy cartilage, this procedure can significantly relieve pain, restore function, and delay the need for a partial or total knee replacement by many years.
Who Is This For?
First 2 weeks
The most important aspects of the initial recovery are controlling swelling in the knee, preventing muscle wasting, and working towards regaining full range of knee motion
The choice depends on where the deformity originates. A High Tibial Osteotomy (HTO) involves cutting the shin bone just below the knee, typically to correct bow-legged (varus) alignment. A Distal Femoral Osteotomy (DFO) involves cutting the thigh bone just above the knee, usually to correct knock-kneed (valgus) alignment. Sometimes, a combined two-level approach is required.
They serve different purposes. An osteotomy preserves your natural joint, making it ideal for younger, active patients who want to return to high-impact activities that might damage a knee replacement. However, it requires a longer initial recovery for the bone to heal compared to a partial knee replacement.
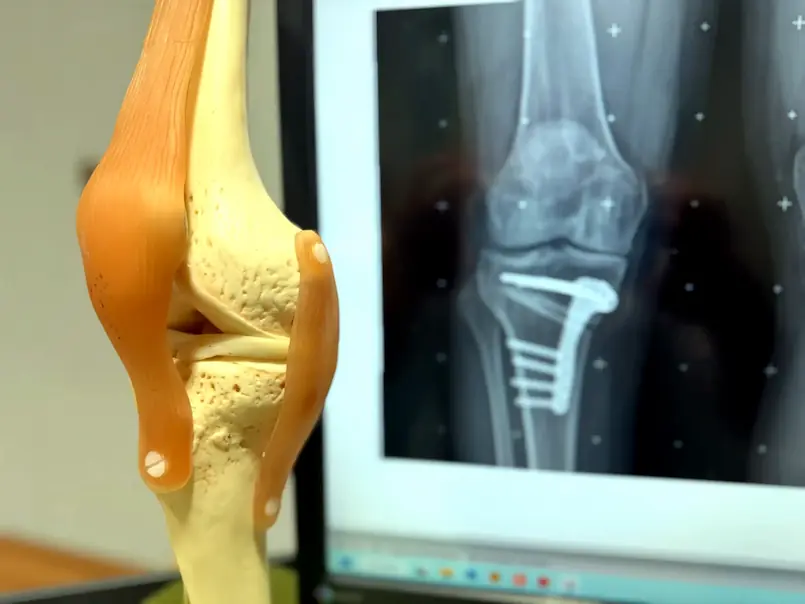
In most cases, the titanium plate and screws are left in place permanently as they do not cause symptoms. However, if the hardware becomes prominent or irritating under the skin (more common in slimmer patients), it can be removed in a minor day-case procedure once the bone has fully healed (usually after 12-18 months).
Clinical studies show excellent long-term results, with 80% to 90% of patients not requiring a knee replacement 10 years after their osteotomy. By correcting the mechanical axis, the progression of arthritis is significantly slowed.
Yes. One of the primary advantages of a realignment osteotomy over a joint replacement is that once the bone is fully healed and rehabilitated, there are generally no permanent restrictions. Many patients successfully return to running, skiing, and high-impact sports.
As with any major bone surgery, there will be discomfort during the initial recovery phase. However, Sven Putnis uses advanced, multimodal pain management protocols during and after the operation to ensure your pain is well-controlled, allowing you to begin early rehabilitation.
Recovery Time
3 to 6 months for full return to unrestricted activity
Hospital Stay
Usually 1 to 2 nights
Success Rate
80-90% survivorship at 10 years (delaying joint replacement)
Book a consultation to discuss if this treatment is right for you.
Book your consultation today and begin your journey to recovery with expert knee care in Bristol.